Services
The Prostate: Anatomy & Function
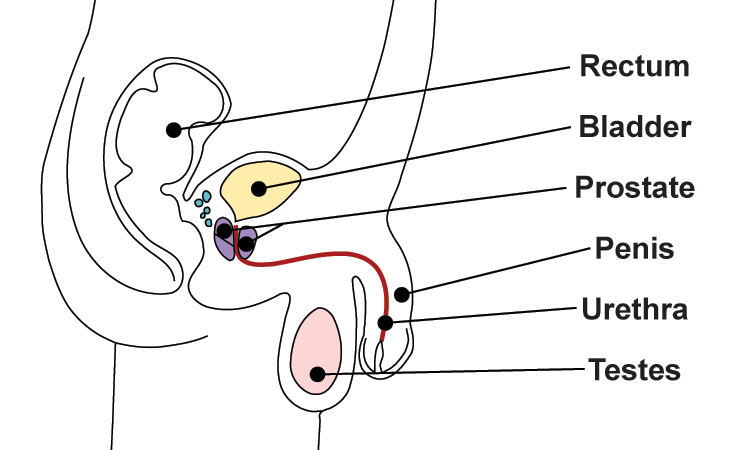
The prostate is a walnut-shaped gland about 1.5 inches long. Located directly beneath the bladder, the prostate completely surrounds the urethra, the channel running from the bladder through the penis, which carries both urine and semen from the body.
The prostate gland's primary function is to produce part of the fluid that makes up semen. During ejaculation, muscles in the prostate contract to push prostatic fluid through tiny ducts into the urethra, where it mixes with sperm and other fluid and is expelled from the body through the penis.
The prostate produces a protein called prostate specific antigen (PSA). PSA is released with the ejaculatory fluid and can also be traced in the blood stream. Testing of PSA levels in the blood is used to detect prostate cancer.
Diagnoses/Treatment
Benign Prostatic Hyperplasia (BPH)
Benign prostatic hyperplasia (BPH) is a non-cancerous enlargement of the prostate gland that occurs in almost all men as they age. This enlargement is usually harmless, but it often results in problems urinating. About half of all men over the age of 50 experience some symptoms.Treatment focuses on reducing symptoms, and is based on how severe symptoms are and whether there are complications. The American Urological Association (AUA) has developed a symptom index to help determine the severity or urinary symptoms, as well as to measure the effectiveness of treatment.
Initial Treatment
The AUA makes the following treatment recommendations for BPH based on the severity of symptoms:- Symptoms that are mild, or that do not bother you (AUA socre of 0 to 7) may be treated by watchful waiting. This means that you may make small lifestyle changes to control symptoms, but that you do not take medications or have surgery. You should have regular checkups to be certain that symptoms are not getting worse.
- Treatment of moderate to severe symptoms (AUA score of 8 or more) depends on how much you are bothered by them. If the symptoms are not greatly affecting your quality of life, you may choose watchful waiting or treatment with medication. If the symptoms are bothersome, or you want more aggressive treatment, you may be offered surgery or less invasive therapies, such as transurethral microwave therapy (TUMT) or transuretheral needle ablation (TUNA).
- Severe symptoms, such as ongoing inability to urinate, bladder stones, kidney damage, or ongoing blood in the urine, should be treated with surgery.
There are some things you can do that may help reduce how much BPH affects your quality of life.
- Do not try to rush urination. Try to relax while using the bathroom.
- Spread your fluid intake throughout the day. Limit fluid intake in the evening if you frequently awaken at night to urinate.
- If possible, avoid medications that make symptoms worse.
- You may want to try an herbal therapy for BPH, such as palmetto or beta-sitosterol, but talk with your doctor first, since these herbal remedies have been proven to be no better than placebos (sugar pills).
Treatment if the Condition Worsens
If any of the following occur, you will probably need surgery for benign prostatic hyperplasia (BPH):- You cannot urinate. About half of men who cannot urinate need catheterization.
- Half of these men will be able to urinate again after catheterization. Those who do not improve may need surgery.
- Your BPH is causing repeated urinary tract infections, bladder stoned or bladder damage.
- You have heavy bleeding in your urine that is not getting better.
- You have kidney damage.
What To Think About
Unless surgery is required due to a complication, choosing a treatment is largely up to you and your doctor. If complications arise, surgery may be necessary.The extent to which treatment improves your symptoms depends partly on the severity of your symptoms and how bothersome they become. If you are not bothered by your symptoms before treatment, you are less likely to notice much improvement after treatment.
Surgery offers the best chance for improving the symptoms but also has the risk of causing other problems.
Benign Hyperplasia (BPH) Surgery
The oldest surgical method to treat BPH is an open prostatectomy, in which an incision is made through the skin to reach the prostate. Doctors use this method less often now, but it is still preferred if the prostate is very large.Surgery that does not require an incision through the skin is usually used. The surgical instruments are passed up the urinary opening in the penis to the location of the prostate. This is described as a transurethral surgery of the prostate. The procedures most commonly performed are:
- Transurethral resection of the prostate (TURP), in which a portion of the prostate is removed.
- Transurethral incision of the prostate (TUIP), in which incisions are made in the prostate that cause it to press less on the urethra.
- Laser therapy (transurethral laser coagulation and tranasurethral laser vaporization), in which a laser is used to make incisions in or remove a portion of the prostate.
- Transurethral needle ablation (TUNA), in which needles are inserted into the prostate, which is then heated with radiofrequency energy and the glandular tissue reduced.
- Transurethral microwave therapy (TUMT), in which microwave energy is used to destroy a portion of the prostate through heating.
- Transurethral electrovaporization of the prostate, in which an electric current is used to destroy a portion of the prostate.
In some cases, these treatments have been studied for only a few years, so their long-term effectiveness is not yet known.
What To Think About
Surgery is the most reliable way to relieve symptoms. However, it may not relieve all symptoms and puts you at risk for certain surgical complications, including erection problems (erectile dysfunction). Other complications include the inability to control the release of urine (urinary incontinence) and ejaculation of semen into the bladder instead of out through the penis (retrograde ejaculation). The complication depends on which type of surgery is used.Men who have severe symptoms often notice great improvement in quality of life following surgery. Men whose symptoms are mild may find that surgery does not greatly improve quality of life, and they may want to think carefully before deciding to have surgery to treat BPH.
If you have decided to have surgery, or if there are clear medical reasons to have surgery, the best surgical option depends on the size and shape of your prostate and the experience of the surgeon.
- Transurethral resection of the prostate (TURP) is the most common surgery for BPH.
- Transurethral incision of the prostate (TUIP) is most effective for men with smaller prostates. It has fewer risks and a shorter recovery period than TURP, and it appears to be nearly as effective in relieving symptoms.
- Transurethral needle ablation (TUNA), in which needles are inserted into the prostate, which is then heated with radiofrequency energy and the glandular tissue reduced.
Transurethral Microwave Therapy (TUMT) for BPH
In transurethral microwave therapy (TUMT), an instrument (called an antenna) that sends out microwave energy is inserted through the urethra to a location inside the prostate. Microwave energy is then used to heat the inside of the prostate. Cooling fluid is circulated around the microwave antenna to prevent heat from damaging the wall of the urethra. To prevent the temperature from getting too high outside the prostate, a temperature sensor is inserted into the man's rectum during the procedure. If the temperature in the rectum increases too much, the treatment is turned off automatically until the temperature goes back down.The temperature becomes high enough inside the prostate to kill some of the tissue. As this part of the prostate heals, it shrinks, reducing the blockage of urine flow.
This treatment is done in a single session. The procedure is performed in the office.
Microwave therapy is also known as cooled thermal therapy or by the name of the equipment (Targis or Prostatron).
Prostate Cancer
Prostate Cancer is a disease in which cancer cells are found in the tissues of the prostate gland. Prostate cancer is more common in men over the age of 50. It is the second most common cause of cancer deaths among men. Prostate cancer may be curable if it is discovered early.The exact cause of prostate cancer is not known, but it is believed that factors such as age and family history may increase the risk of developing the disease.
Symptoms
Prostate cancer usually does not cause symptoms in its early stages. When there are symptoms, they may include:- Hesitancy, or difficulty starting a urine stream
- Weaker-than-normal urine stream
- Inability to urinate at all
- Having to urinate often
- Feeling that the bladder is not emptying completely when urinating
- Getting up at night to urinate. This is called nocturia.
- Pain or buring during urination. This is called dysuria.
- Blood in the urine. This is called Hematuria.
- Blood in the semen. This is called hematospermia.
- Deep pain in the lower back, abdomen, hip or pelvis
These symptoms may also be caused by:
- Benign Prostatic Hyperplasia (BPH), which is an enlarged prostate. This is very common in older men. The prostate usually grows larger with age. When it gets large enough, it can press against the urethra--the tube that carries urine from the bladder through the penis--and cause bladder problems.
- Prostatitis, an infection in the prostate
- Urinary Tract Infection, an infection in any of the organs that make urine or the tubes that carry it out of the body.
Symptoms that may indicate the cancer has spread, or metastasized, to other parts of the body include:
- Weight loss
- Bone pain, especially in the lower abdomen, hip, pelvis or lower back
- Swelling in the legs and feet